Study population
A total of 214 patients in CKD 4-5 stages between June 2021 and June 2024 were included in the study. The diagnosis and staging of CKD were conducted in accordance with the Clinical Practice Guidelines for Chronic Kidney Disease13. These patients demonstrated sinus rhythm during their echocardiographic evaluations. Exclusion criteria Cardiomyopathies (diseases causing left ventricular wall thickening such as hypertrophic cardiomyopathy, Fabry disease, cardiac amyloidosis, etc.), myocardial infarction, and coronary artery atherosclerosis. Additionally, significant valvular heart diseases (at least mild valve stenosis, moderate or severe aortic or mitral regurgitation, severe pulmonary or tricuspid regurgitation), congenital heart diseases, and individuals unable to cooperate with echocardiographic examinations or with poor image quality were excluded.
Finally, A total of 173 CKD patients met the inclusion criteria and were included in the analysis. They were categorized into two groups based on the presence or absence of DM, the CKD-DM group (n = 98) and the CKD + DM group (n = 75) (Fig. 1). The diagnosis of type 2 diabetes mellitus (T2DM) was established according to the guidelines provided by the American Diabetes Association or the use of antidiabetic medications14. The clinical endpoint in this study is the occurrence of MACE, a composite outcome encompassing all-cause mortality or hospitalization due to heart failure. Hospitalization for heart failure is specifically defined as admission necessitated by heart failure symptoms that mandate intravenous diuretic therapy. The methods employed in this study were conducted in strict adherence to applicable guidelines and regulations. This study was approved by the Ethics Committee of Guizhou Medical University Affiliated Hospital (Ethics Approval No: [2021] Ethics Approval Department 318). It was conducted as a retrospective study, and informed consent was waived.
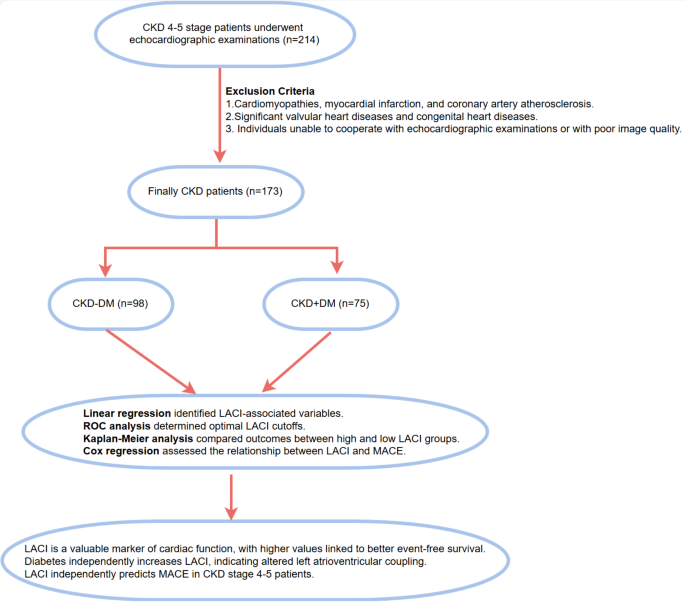
Data collection of demographics and laboratory measurements
Relevant demographic information, encompassing age, gender, height, weight, body surface area (BSA), systolic blood pressure (SBP), diastolic blood pressure (DBP), smoking history, alcohol consumption history, and diabetes history, dialysis history, and stage of CKD was meticulously retrieved from the patients’ medical records. The collection of laboratory data involved the assessment of cardiac biomarkers, including Troponin T, Myoglobin, and N-terminal pro-brain natriuretic peptide (NT-proBNP). Additionally, renal function indicators, such as Urea, Creatinine, Uric acid, Cystatin C, and estimated glomerular filtration rate (eGFR), were also included.
Echocardiography
The echocardiographic assessment was conducted using the Philips EPIQ7C and Philips EPIQCVx color Doppler ultrasound systems, equipped with an X5-1 transducer (frequency range: 1–5 MHz). Acquire high-quality and dynamic DICOM images of the apical four-chamber, three-chamber, and two-chamber views of the heart in accordance with the guidelines15, Data were obtained by averaging measurements from five consecutive stable cardiac cycles, then store them on the hard drive. A comprehensive analysis of echocardiographic parameters, including two-dimensional imaging, doppler measurements, and tissue doppler assessments, was performed by experienced sonographers with a minimum of 10 years of expertise. The following key parameters were measured: left ventricular end-diastolic diameter (LVEDD), left ventricular end-diastolic volume (LVEDV), LVEF, left ventricular mass (LVM), left atrial anteroposterior diameter (LAD), left atrial end-diastolic volume (LAEDV), interventricular septum (IVS) and left ventricular posterior wall (LVPW) thickness, early and late diastolic peak velocities across the mitral valve (E, A), mean velocities of early diastolic septal and lateral mitral annular motion (e′), calculated E/A ratio, E/e′ ratio, LVMI and LAEDVI were derived by normalizing the measurements with respect to the BSA.
Subsequently, 2D speckle tracking imaging (2D-STI) was performed. LA and LV views were acquired with appropriate image magnification in the apical four-chamber view. Automated myocardial motion tracking and region of interest (ROI) generation were conducted using the QLAB 13 quantitative analysis software. The software automatically derived several temporal strain values for the LA and LV, including left atrial reservoir strain (LASr), left atrial conduit strain (LAScd), left atrial contraction strain (LASct) and left ventricular global longitudinal strain (LVGLS). The left atrial stiffness index (LASI) was calculated as E/e′/LASr, and LACI was determined as LAEDV/LVEDV. Measurements of LA and LV volumes were obtained at the same diastolic phase. A higher LACI indicates a greater disparity between LV volume and LA volume at end-diastole, which reflects a more significant impairment in left atrioventricular coupling11.
Reproducibility analysis
To assess the variability within and between observers, a randomized sample of 10 subjects was selected from each study group. Two ultrasound physicians, each possessing more than 10 years of professional experience, independently conducted measurements of LA and LV strain, LVEDV, LAEDV for the selected subjects. Following a two-week interval, the same ultrasound physicians reexamined the selected cases. Intra-observer variability was evaluated by utilizing the two sets of measurements obtained by the first investigator, whereas inter-observer consistency was assessed based on the results derived from the two physicians.
Statistical analysis
Categorical data in this study were presented as frequencies (%). Group comparisons were conducted using the chi-square test. The normality of continuous variables was assessed using the Shapiro-Wilk test. Normally distributed continuous variables were reported as mean ± standard deviation (SD), while non-normally distributed variables were presented as median (interquartile range). Group comparisons of continuous variables were performed using independent-samples t-test or Mann-Whitney U test, as appropriate. Spearman’s correlation coefficient was utilized to evaluate the correlation between clinical and ultrasound parameters in CKD patients. Multiple linear regression analysis was conducted to evaluate the factors influencing the LACI. Variables that demonstrated significance (p < 0.05) in the univariate analysis were included in the multivariate model, with a variance inflation factor of 5 applied to mitigate multicollinearity. The Receiver Operating Characteristic (ROC) curve was utilized to compute the area under the curve (AUC), determining the optimal LACI cut-off value for MACE prediction. Kaplan-Meier survival curves and log-rank tests were used to compare event-free survival rates between patients with high and low LACI values. A multivariate Cox proportional hazards regression model was utilized to identify independent predictors of MACE, encompassing covariates that were statistically significant or clinically relevant in the univariate analysis, with outcomes expressed as hazard ratios and 95% confidence intervals. Intra-observer and inter-observer variability of LASr, LAScd, LASct, LVGLS, LAEDV, and LVEDV were evaluated using the Interclass Correlation Coefficients (ICC). Statistical analysis was conducted using IBM SPSS Statistics 25.0 software. A two-tailed p-value less than 0.05 was considered statistically significant. GraphPad Prism software (version 8.0) was used to draw the heat map, ROC curve and the Kaplan-Meier survival curves.
link











More Stories
Russia turns to high altitude balloons after Starlink restrictions disrupt battlefield communications across Russian-controlled territories
What CES 2026 didn’t show: The quiet crisis in wireless capacity nobody is talking about
Recent AWS issues blamed on AI tools – at least two incidents affected some Amazon services